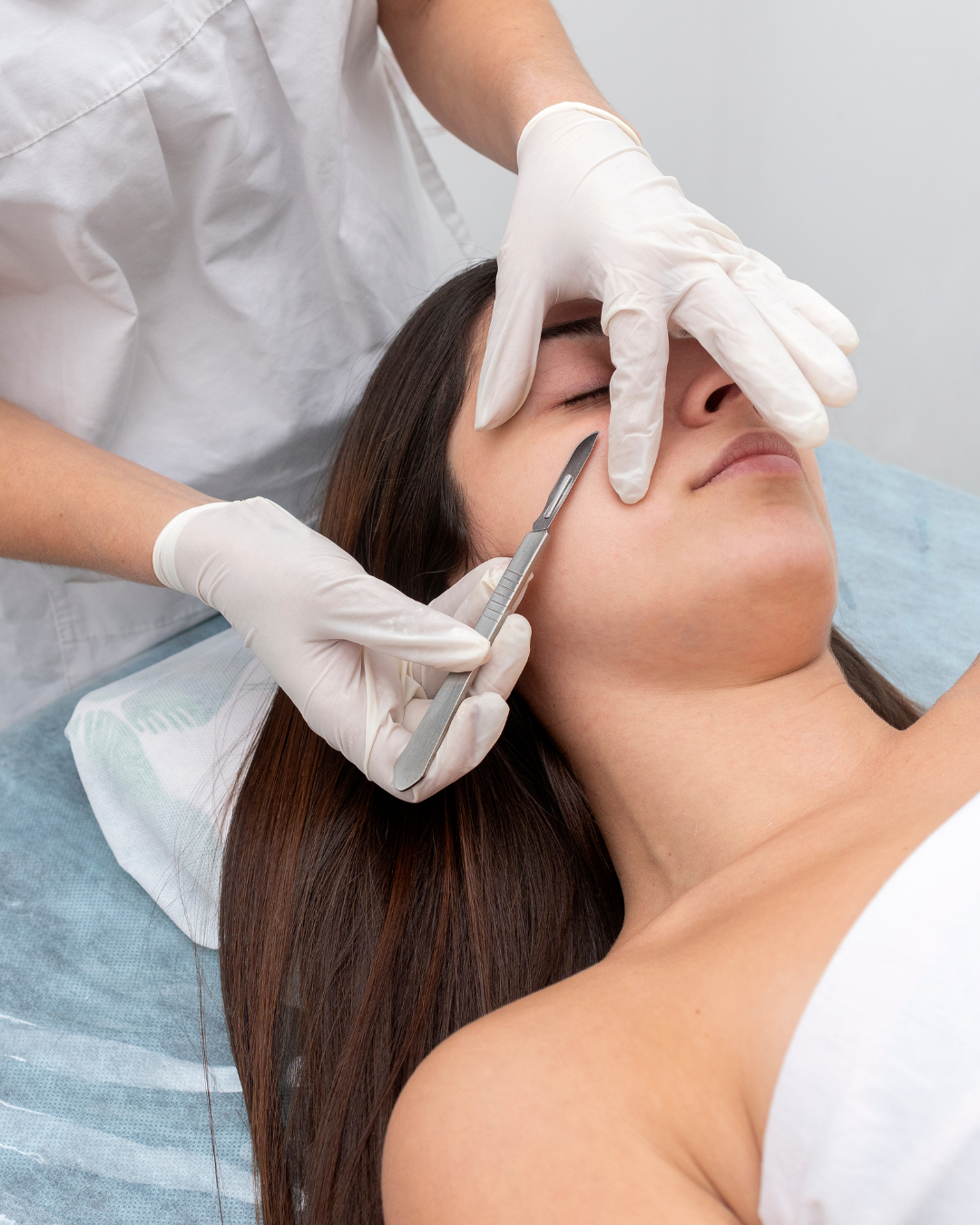
Dermaplaning Complications: What Professionals Should Know (Clinical Safety Guide 2026)
Dermaplaning is often marketed as a simple exfoliation treatment — but in professional practice, it requires precision, anatomical knowledge, and strict infection control.
While dermaplaning is generally low-risk when performed correctly, improper technique, poor screening, or sanitation lapses can lead to complications.
For licensed estheticians in Colorado, understanding potential risks is essential for protecting clients, maintaining compliance with DORA regulations, and safeguarding your professional reputation.
This guide outlines the most common dermaplaning complications, how to prevent them, and when referral is appropriate.

Why Complication Awareness Matters
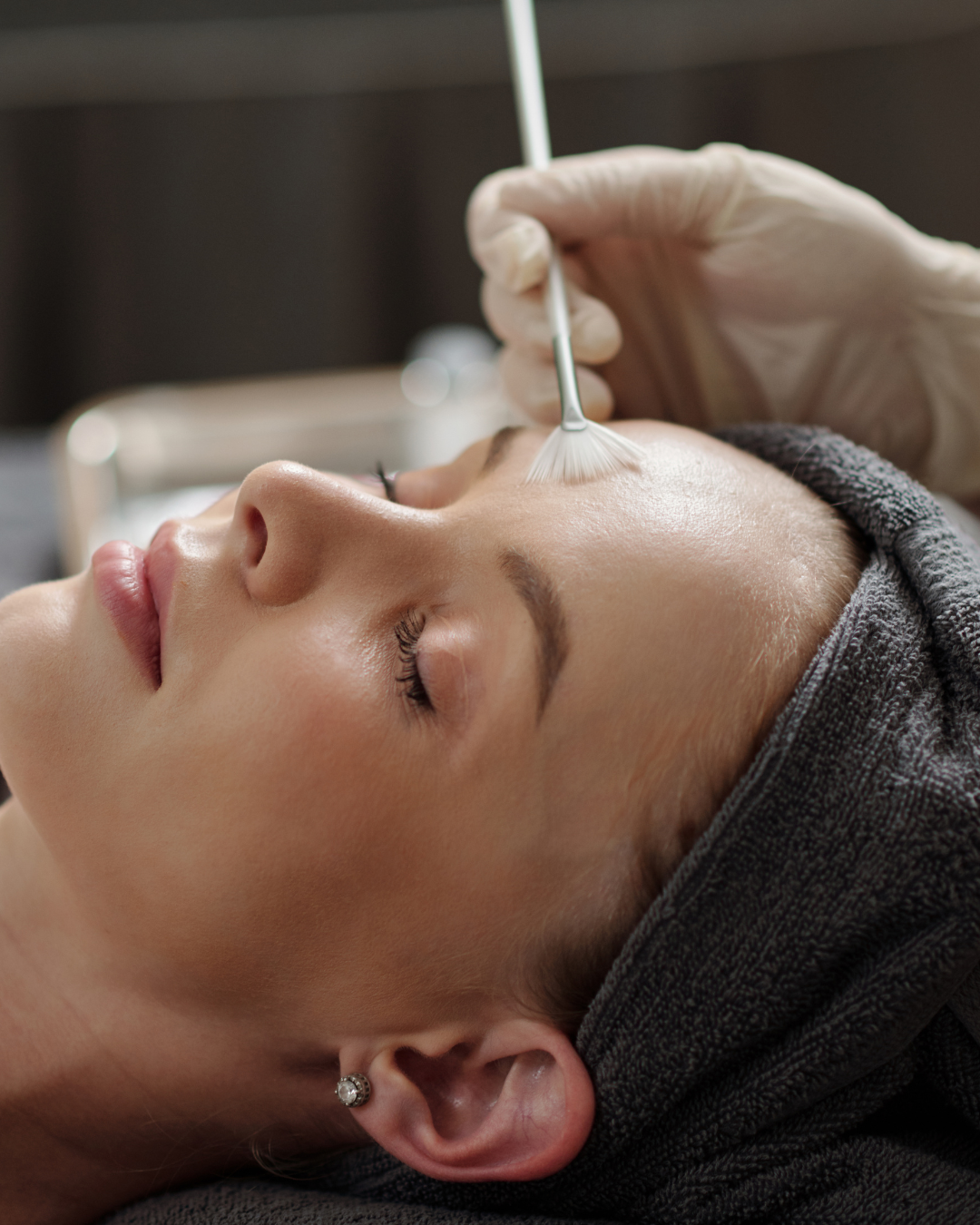
Dermaplaning involves controlled removal of the outermost layer of dead skin cells using a sterile blade. Even though the treatment is superficial, you are still:
Using a sharp instrument on the skin
Creating controlled exfoliation
Temporarily increasing skin sensitivity
The difference between a smooth result and a complication often comes down to:
Proper client selection
Correct blade angle
Pressure control
Skin tension technique
Post-treatment education
Advanced training reduces risk — but professional judgment prevents complications.
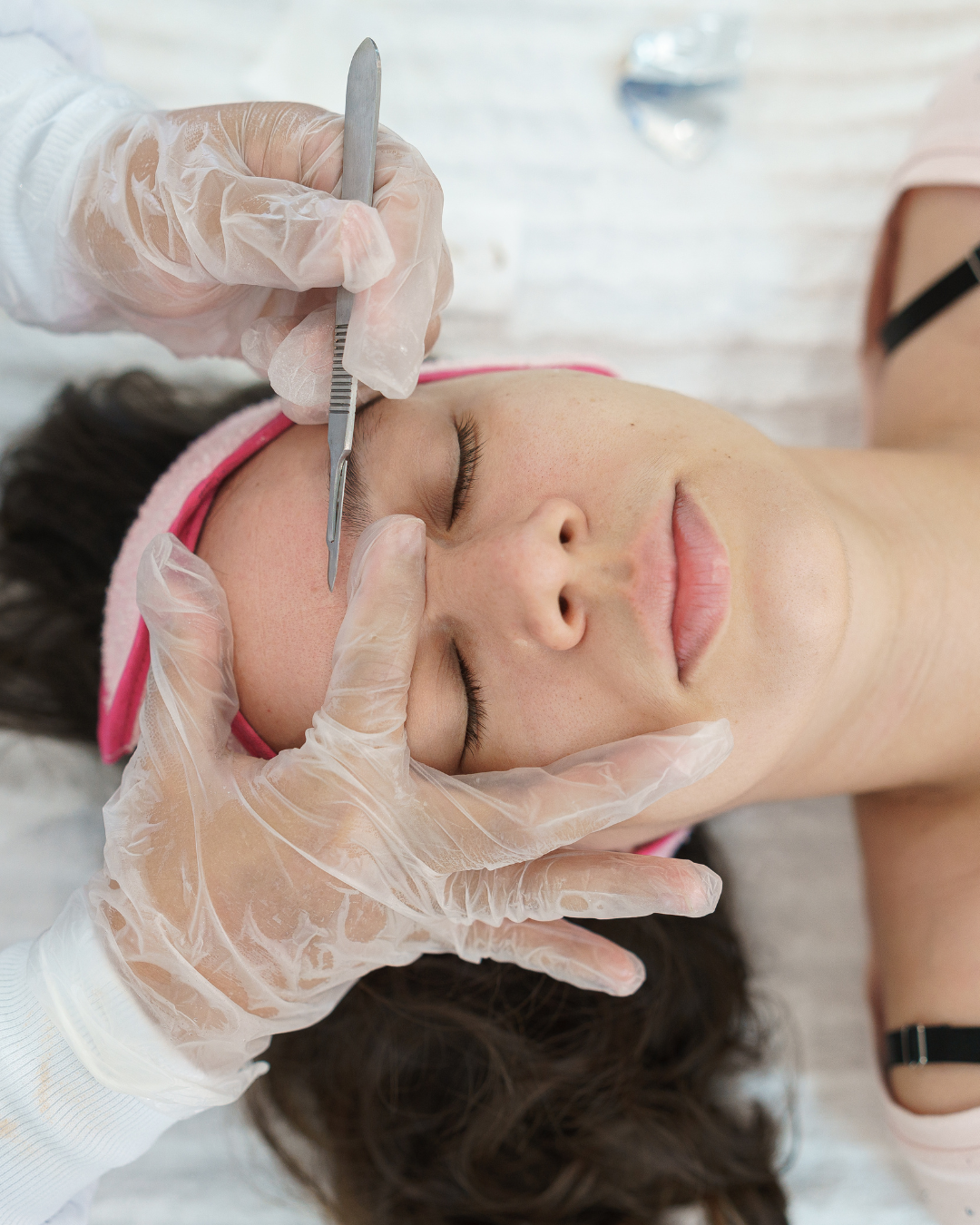
Most Common Dermaplaning Complications
Surface Nicks or Abrasions
Small cuts are the most common technical complication.
Causes:
Incorrect blade angle
Excess pressure
Insufficient skin tension
Working over uneven or inflamed areas
Prevention:
Maintain approximately a 45-degree blade angle
Use light, feathered strokes
Avoid raised lesions or active acne
Stretch skin properly before each pass
Proper blade control comes from hands-on repetition under supervision.
Breakouts After Treatment
Some clients experience post-treatment breakouts.
Causes:
Treating active acne improperly
Cross-contamination
Inadequate blade sterility
Occlusive products applied post-treatment
Prevention:
Avoid dermaplaning over inflamed acne lesions
Follow strict sanitation protocols
Use sterile, single-use blades
Choose non-comedogenic post-care products
Proper client screening significantly reduces breakout risk.

Irritation & Barrier Sensitivity
Because dermaplaning removes superficial dead skin cells, the skin barrier becomes temporarily more sensitive.
Signs:
Prolonged redness
Tightness
Stinging when applying products
Causes:
Overworking the same area
Excessive pressure
Combining with aggressive exfoliants
Prevention:
Limit repeated passes over the same zone
Avoid pairing with strong acids unless properly trained
Emphasize barrier-repair homecare
Conservative technique protects the skin’s integrity.
Post-Inflammatory Hyperpigmentation (PIH)
Although less common than with chemical peels, dermaplaning can contribute to PIH if inflammation occurs — especially in higher Fitzpatrick skin types.
Causes:
Aggressive pressure
Working on sensitized skin
Inadequate sun protection post-treatment
Prevention:
Assess Fitzpatrick skin type
Avoid overly aggressive strokes
Require strict SPF compliance
Delay treatment if barrier is compromised
Gentle technique is critical in melanin-rich skin.
Infection
Infection is rare when sanitation is followed properly — but possible.
Causes:
Improper blade disposal
Reusing blades
Inadequate disinfection of treatment area
Treating open wounds
Prevention:
Use sterile, single-use blades only
Follow sharps disposal regulations
Disinfect all surfaces thoroughly
Avoid treatment on broken skin
Infection always requires medical referral.
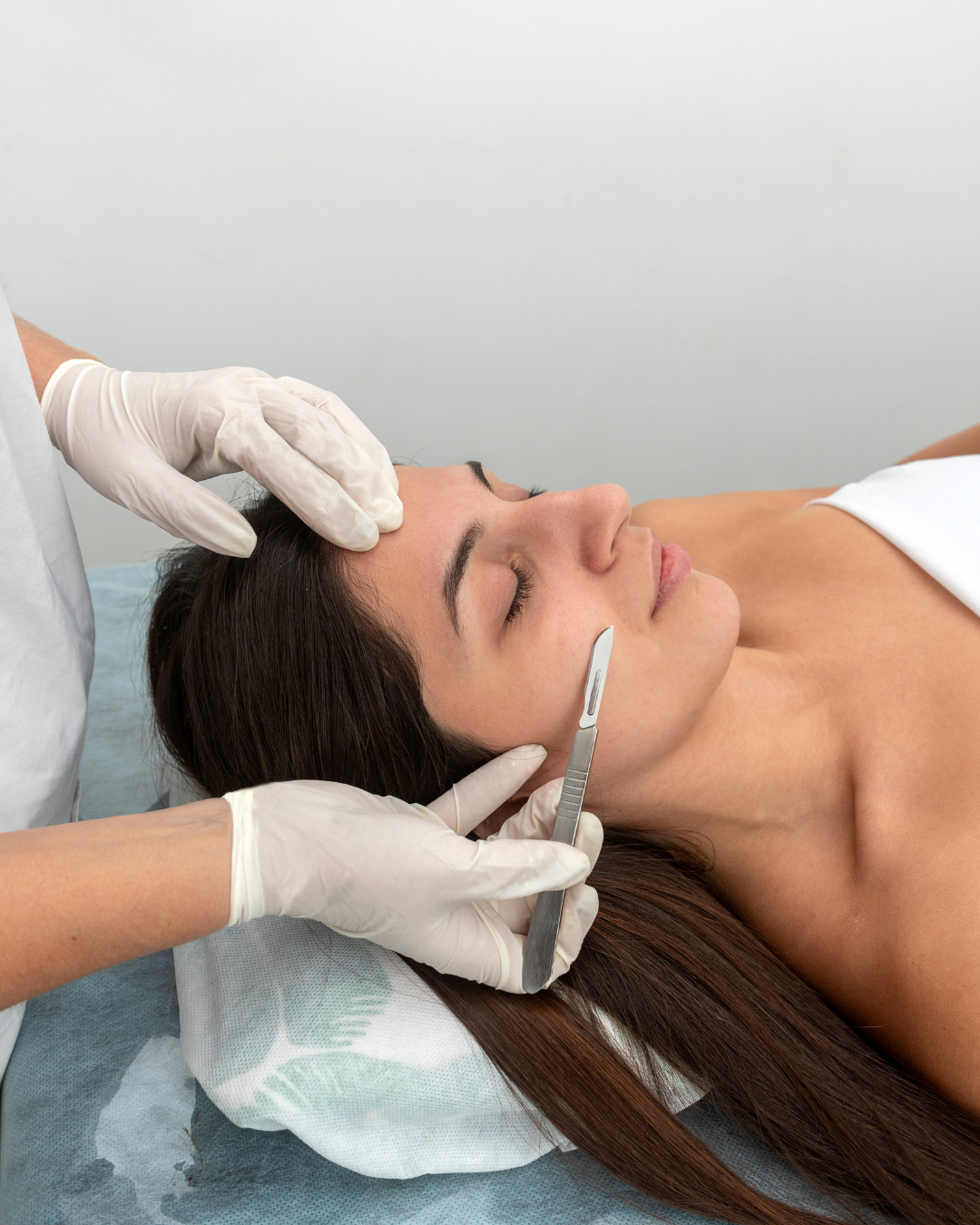
Contraindications That Increase Risk
Professionals should carefully screen for:
Active acne with pustules
Rosacea flare-ups
Open lesions or wounds
Compromised barrier
Recent laser or chemical peel procedures
Recent isotretinoin use
Treating contraindicated skin increases complication likelihood.
Scope of Practice in Colorado
Dermaplaning falls under esthetic practice in Colorado and is regulated by the Department of Regulatory Agencies (DORA).
Licensed estheticians may perform non-invasive exfoliation services, including dermaplaning, within their scope of practice. However:
Procedures must remain cosmetic in nature
Infection control standards must be followed
Practitioners must avoid medical-level interventions
Operating outside scope not only increases clinical risk but may also lead to disciplinary action.
Documentation & Risk Management
Professional dermaplaning practice should include:
Written consultation forms
Contraindication screening checklist
Informed consent
Pre-treatment photos
Detailed treatment notes
Clear aftercare instructions
Thorough documentation protects both practitioner and client.

When to Refer to a Medical Provider
Referral is appropriate if you observe:
Signs of infection
Persistent swelling
Unexpected pigmentation changes
Delayed healing
Excessive inflammation
Knowing when to refer demonstrates professionalism and protects your license.
How Advanced Training Reduces Complications
High-quality dermaplane certification teaches professionals to:
Control blade angle precisely
Maintain proper skin tension
Screen for contraindications effectively
Combine treatments conservatively
Recognize early warning signs
Operate within Colorado scope-of-practice regulations
Dermaplaning may appear simple — but safe mastery requires structured education.
Final Takeaway
Dermaplaning complications are preventable when professionals combine:
Strong foundational knowledge
Careful client screening
Conservative technique
Strict sanitation
Ongoing education
In advanced esthetics, safety awareness separates hobby-level practice from professional expertise.
Elite Aesthetics Academy’s Dermaplane Training Program in Denver emphasizes hands-on blade control, complication prevention, and regulatory compliance to ensure graduates practice confidently and responsibly.
Precision and professionalism protect both your clients and your career.
👉 Explore 600-hour esthetician license program in Denver




